Our Health Cause
Our health programmes are primarily focused on providing support for the total health and well-being of target beneficiaries to help them thrive. According to WHO, total health and well-being encompass the physical, mental and social well-being, and not merely the absence of diseases.
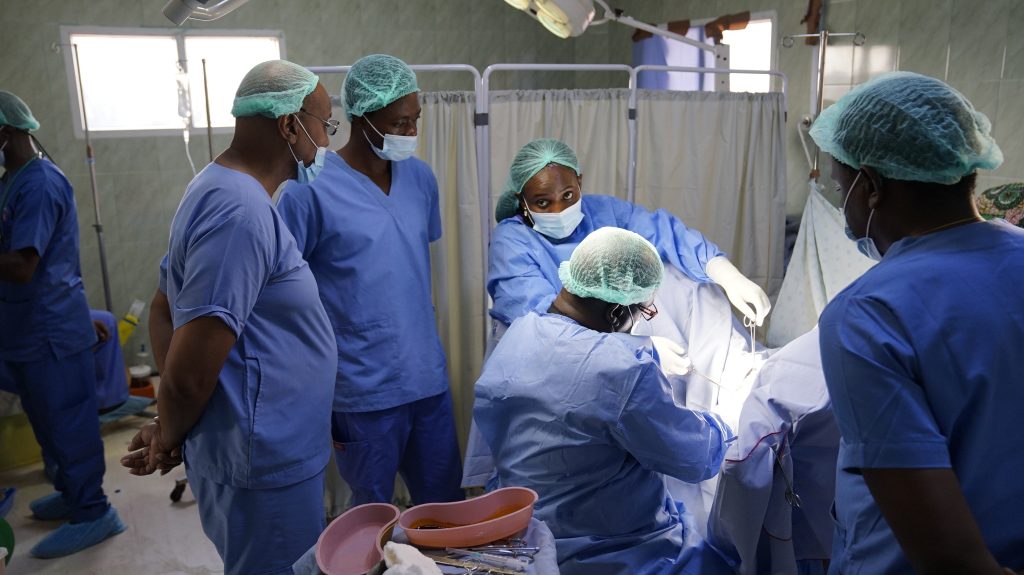
UBOMI Medical & Surgical Outreach
UBOMI which means “Life”, is a free medical and surgical outreach held in line with the Global Sustainability Development Goal to ensure healthy lives and promote well-being for all at all ages.
It is held each year in target communities including but not limited to Eti-Osa (Jakande, Ajah), Mainland (Maryland) etc. It provides medical, surgical, dental, eye, pharmaceutical and laboratory services, amongst other things, to underserved members of the communities in which it is held.
Other Health Programmes
Preventative and Curative Initiatives
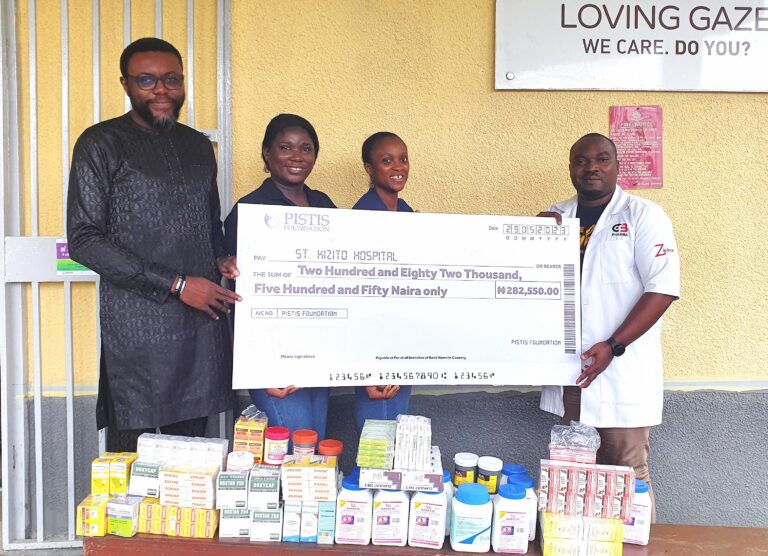
Medical Grants & Partnerships
One-off medical grants (for economically challenged people) are available for primary health concerns or cases requiring urgent medical attention. These interventions are usually carried out in collaboration with partner medical institutions who support our goal to meet needs in our target communities.

Health Campaigns
Pistis Foundation’s preventative strategy aims to positively influence the health behaviour of individual and communities, as well as the living and working condition that influence their health. This is achieved through online campaigns, webinars and health awareness walks.

